Living with diabetes requires closer attention to foot health, not only for comfort, but to prevent potentially serious complications. Even a small blister, minor cut, or pressure spot can develop into a diabetic foot ulcer if it goes unnoticed or untreated. Diabetes can reduce blood circulation and impair nerve function, which slows wound healing and makes infections easier to develop and spread. This is why early and proactive podiatry care is essential to protect mobility, maintain independence, and support long-term quality of life.
Encouragingly, up to 80% of diabetic foot ulcer cases can heal successfully with appropriate treatment from a podiatrist. Early assessment and structured care are crucial to preventing avoidable complications and preserving limb health. Read the full article and learn more — perhaps it’s your time to seek professional podiatry care at My Foot Dr Singapore.
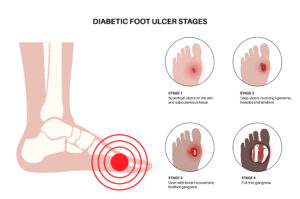
What Is a Diabetic Foot Ulcer?
A diabetic foot ulcer is an open sore or wound that most commonly develops on the sole of the foot in people living with diabetes. It occurs when the skin breaks down and exposes the tissue underneath, creating a wound that can deepen if not treated promptly. This condition affects an estimated 15% of individuals with diabetes and is considered one of the most serious diabetes-related foot complications.
Diabetic foot ulcers are often underestimated in their early stages, as mild redness, small cracks, or minor skin damage may appear harmless. However, overlooking these warning signs can lead to serious consequences. Without timely care, ulcers can worsen quickly, become infected, and in severe cases, result in hospitalisation or limb amputation. Prompt assessment and treatment by a podiatrist or specialised wound care team are essential to prevent complications, control infection, and protect long-term foot health.
Common Causes of Diabetic Foot Ulcers
Diabetic foot ulcers usually develop from a combination of medical and lifestyle factors that affect how the feet sense pressure, heal wounds, and tolerate daily stress. Diabetes can damage nerves and blood vessels, alter foot structure, and weaken the body’s ability to repair skin injuries. As a result, even small wounds or repeated friction can gradually progress into serious open sores if not properly managed.
Key Contributing Factors
- Peripheral neuropathy (nerve damage): Reduced sensation in the feet makes it difficult to feel pain from cuts, pressure, heat, or friction. Minor injuries can go unnoticed and worsen over time. Nerve damage may also weaken foot muscles, leading to deformities that create high-pressure areas.
- Peripheral artery disease (poor circulation): Reduced blood flow limits oxygen and nutrient delivery to tissues, slowing wound healing and increasing the risk of infection and tissue damage.
- Foot deformities: Structural changes such as bunions, hammertoes, or Charcot foot create abnormal pressure points that are highly prone to skin breakdown and ulcer formation.
- Repeated pressure or friction: Ongoing rubbing from tight, loose, or unsupportive footwear can damage the skin and underlying tissue.
- Minor trauma: Small cuts, blisters, puncture wounds, or cracked skin can develop into ulcers when not detected and treated early.
- Callus build-up: Thickened skin often signals excessive pressure on specific areas of the foot, where ulcers commonly form beneath the surface.
- Poor blood sugar control: Elevated glucose levels weaken immune response and delay the body’s natural healing processes.
- Previous ulcers or amputation history: Past foot complications significantly increase the likelihood of recurrence.
When Should You See a Podiatrist?
If you are living with diabetes, any change in your foot health should be taken seriously. Diabetes can reduce blood circulation and damage nerves, which means wounds heal more slowly and pain signals may be dulled or absent. As a result, minor cuts, blisters, pressure spots, or skin changes can quietly worsen into serious complications.
Early podiatry assessment ensures problems are properly diagnosed, treated at the right stage, and prevented from progressing into infections or ulcers that threaten mobility and limb health. Recognising these warning signs early allows timely treatment before complications develop. Prompt podiatry care helps protect tissue health, prevent infections, and maintain safe, confident movement.
Seek professional podiatry care if you notice:
- A wound or sore that does not improve within a few days
- A sore that becomes larger, deeper, darker, or discoloured
- Redness, swelling, unusual warmth, or fluid discharge
- Open skin or ulcers, even when there is no pain
- Recurrent calluses or repeated skin breakdown in the same area
- Persistent numbness or reduced sensation in the feet
- Tingling, pricking, or stabbing nerve-like pain
- Unusual foot odour that may signal a hidden infection
How Podiatrists Treat Diabetic Foot Ulcers
Podiatrists provide specialised, primarily non-surgical care that focuses on creating the ideal environment for wound healing, relieving pressure on the affected area, controlling infection, and preventing recurrence. Because every ulcer differs in depth, location, circulation status, and infection risk. Appropriate treatment plans are highly individualised and often involve ongoing follow-up. Diabetic foot ulcer treatment is often a longer-term process that requires regular reviews, dressing changes, and active patient participation. With consistent podiatry care and proper management, healing outcomes improve significantly while the risk of complications is greatly reduced
Wound Debridement
Podiatrists carefully remove dead, damaged, or infected tissue and surrounding callus from the wound. This professional procedure helps reduce bacterial load, encourages healthy tissue growth, and supports faster healing.
Pressure Offloading
Reducing pressure on the ulcer is essential. Depending on severity and mobility needs, podiatrists may recommend specialised medical footwear, diabetic walkers, removable cast boots, protective padding, or mobility aids. In certain cases, total contact casting may be used to redistribute weight more evenly across the foot.
Custom Orthotics and Footwear Guidance
Medical-grade insoles and properly fitted footwear improve foot alignment, reduce friction, and prevent excessive pressure that can worsen wounds or trigger new ulcers.
Custom Shoes
Podiatrists can design custom footwear to effectively manage pressure, helping to redistribute and balance weight across the feet for better protection and comfort. They are especially beneficial for individuals who have had amputations, as they help lower the risk of repeated ulcers and further complications.
Infection Management
Moisture-Balanced Wound Dressings
Podiatrists carefully select wound dressings based on the ulcer’s condition, including its depth, moisture level, and risk of infection. These dressings help maintain an optimal moist environment, control excess drainage, and protect the surrounding tissue to support faster and more effective healing.
Management of Underlying Health Factors
Healing outcomes improve significantly when underlying causes are properly managed. Podiatrists guide patients to monitor their blood circulation, maintain optimal blood sugar levels, and address diabetes-related complications that may slow recovery and wound healing.
How to Prevent Diabetic Foot Ulcers
Preventing diabetic foot ulcers is far more effective than treating them after they develop. Consistent daily foot care, proper diabetes management, and regular professional monitoring greatly reduce the risk of wounds, infections, and serious complications. Small protective habits can make a meaningful difference in preserving long-term foot health and mobility.
- Inspect your feet daily for cuts, blisters, redness, swelling, or colour changes, including the soles and between the toes
- Maintain good blood sugar control to support circulation, nerve health, and wound healing
- Practise proper foot hygiene by washing and drying feet thoroughly each day, especially between the toes
- Moisturise dry skin to prevent cracking, but avoid applying lotion between the toes
- Trim toenails carefully to reduce the risk of ingrown nails and skin injury
- Wear well-fitted, cushioned footwear at all times and avoid walking barefoot, even indoors
- Seek professional podiatry care for nail trimming, corns, or calluses instead of self-treating
- Attend regular podiatry assessments, especially if you are at moderate to high risk
Book Diabetic Foot Ulcer Treatment at My Foot Dr Podiatry Clinic
Professional podiatry care plays a vital role in the safe and effective prevention and management of diabetic foot ulcers. A trained podiatrist can identify early warning signs, deliver precise wound care, and design personalised foot management plans to minimise future risks. Prompt treatment not only supports faster healing but also helps preserve mobility, independence, and overall quality of life.
At My Foot Dr Podiatry Clinic Singapore, our experienced podiatrists provide thorough diabetic foot assessments, advanced wound management, and preventive care tailored to every patient’s condition and lifestyle needs. If you notice foot wounds, skin changes, numbness, or discomfort, schedule a consultation today and take proactive steps to safeguard your foot health!