Diabetic Footcare

Explaining Diabetes
Diabetes is a systemic metabolic disorder that impairs the body’s ability to absorb glucose from the blood stream and provide it to the tissue cells that require it for normal activity and health. The elevated blood glucose levels that remain in the bloodstream produce toxins that affect all body organs and systems, including the circulatory system and the peripheral nerves of the lower limb.
In simple terms, this accelerates the natural ageing process of the lower limb circulation reduction (peripheral vascular disease – PVD), and the loss of normal protective sensation to the foot and leg (peripheral neuropathy) and an inability to fight infection via an impaired immune system. This process does not affect everybody the same way or with the same severity. Research has shown that strict adherence to medical care management, correct nutrition and regular exercise helps to stabilise blood glucose levels and is, therefore, the best way to avoid these complications.
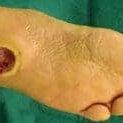
Complications of Diabetes
Initially, changes may be minimal such as noticing dryness of the skin around the toes, or tingling of the toes at night. Eventually this may progress to complete numbness along the sole of the foot, which results in loss of protective sensation and eventually neuropathic ulceration. Reduced circulation to the feet and lower limbs further impacts on these neurological changes and prevents adequate oxygenation and nutrition to the extremities. You may have heard that some people with advanced diabetes progress to foot or leg amputation, and this is a real threat if overall management is not adequate.
What Can Be Done?
Diabetes Australia recommends an annual review by a qualified podiatrist to quantify your foot health status, and the level of risk and precaution you should take. As specialists in this field, podiatrists are able to use diagnostic tests to assess your sensation, circulation and biomechanical risk factors and place that within the bigger picture of your overall health. Furthermore, a podiatrist will provide necessary care management at the time of the consultation involving skin and nail care for corns, calluses or ingrown toenails or ulcer debridement in more advanced cases. Information about your foot health can then be forwarded onto your General Practitioner or specialist Endocrinologist, where further care management can be recommended if necessary.
In addition to regular podiatry assessment and care management, you can do these simple things to take care of your feet:
- NEVER walk barefoot.
- Wash and dry feet thoroughly daily, particularly the area between the toes.
- Visually examine your feet daily to ensure there are no marks, spots, cuts, swelling or redness that are not normal. (Tip: if you have difficulty getting your leg up to see the sole of your foot, a well placed mirror may be of help.)
- Choose correctly fitted shoes with adequate depth and width for the toes. Check the inside of your shoes for foreign objects before you put them on.
- Ensure that socks and stockings are not worn too tightly. Cotton socks with no elastic in the tops will absorb sweat and reduce pressure at the top of the sock line.
- Cut your toenails straight across carefully with good quality nail nippers and file afterwards.
- Moisturise your feet daily, but avoid moisturising in between your toes.
- Have any corns and calluses manageed by a podiatrist. NEVER use over-the-counter corn pads or razor blades.
- Keep your feet away from direct heat including heaters, hot water bottles, scalding hot showers/baths and electric blankets.
- Enjoy exercise and try to be generally active while taking care to prevent injury.
- Attend an annual Podiatry Diabetes Foot assessment.
Regular podiatric care plays an integral role in the prevention of diabetic foot complications.
Routine podiatric care has been shown to decrease the likelihood of limb amputation due to the complications of diabetes.
