If you think that having diabetes is just about controlling your blood sugar levels, think again. Our body is made out of interconnected systems and chronic disease is more likely to cause complications from top to toe. One of such complications is a diabetic foot ulcer.
A diabetic foot ulcer is a condition that commonly plagues diabetic patients. It can cost $8000 for care management. However, if the necessary steps are taken in the early stages, the costs are substantially lower.
But, good news – with prompt care management, up to 80% of the diagnosed cases can recover!
Hence, it is important to know how to recognise the symptoms in advance and why you should not brush them off as a minor complication.
What is a Diabetic Foot Ulcer?
Diabetic foot ulcers are open sores or wounds that are usually located at the bottom of the foot and affect approximately 15 per cent of diabetic patients. This condition is also the most common cause of non-traumatic lower extremity amputation globally and diabetic patients are more susceptible to be at risk.
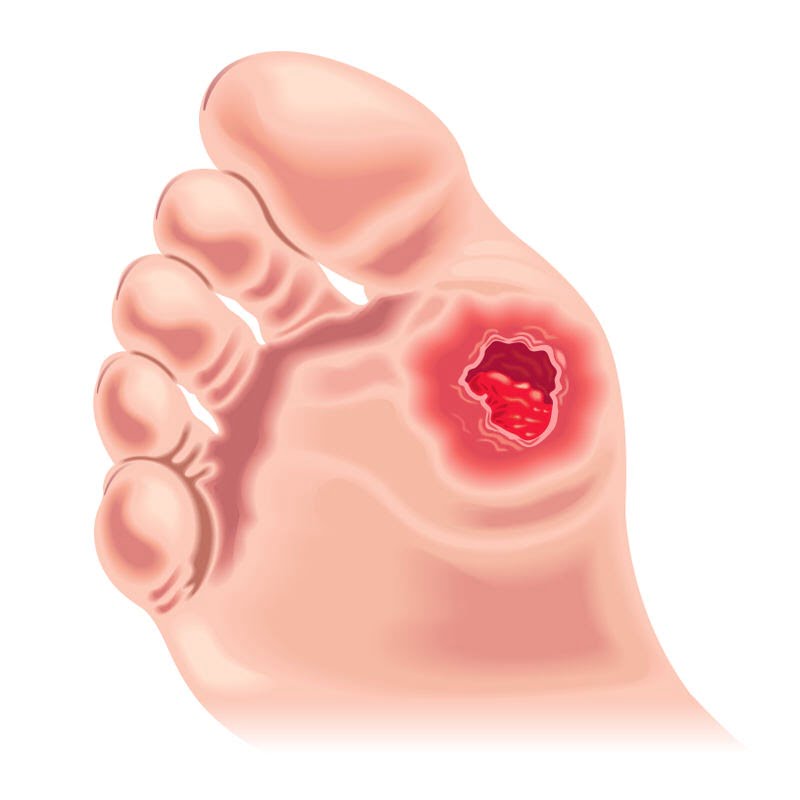
What Causes This Condition?
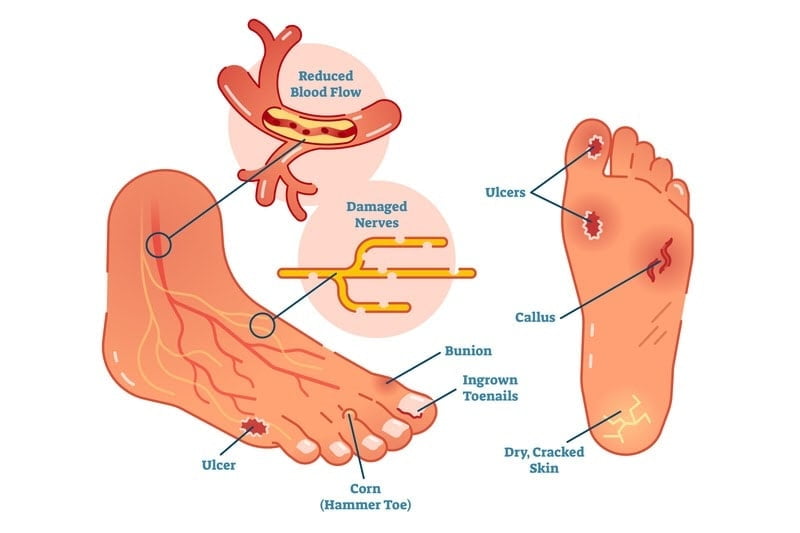
The first cause of foot complications in a diabetic patient is nerve damage from diabetes, causing numbness, and a lack or total loss of feeling in the foot and leg. Also known as peripheral neuropathy caused by chronically high blood sugar damages nerves, hence reducing their ability to carry signals between the brain and other parts of the body.
Without proper signalling, loss of sensation occurs in a part of the body such as the foot, which means the patient becomes unaware of any blisters, ulcers, or even undetected bone fractures.
Vascular disease is another major condition that happens in diabetics and affects the blood vessels supplying the skin, or medically known as microangiopathy. Diabetic patients tend to have narrower arteries, which affects the blood supply to the feet. Thus, a lack of healthy blood flow may cause ulceration and impaired wound healing.
Symptoms of a Diabetic Foot Ulcer
As diabetic foot ulcers are not often seen as a threat, their symptoms are usually dismissed as trivial. However, the fact of the matter is, these symptoms can have severe consequences if ignored and left unmanageed:
-
Numbness
This is the most familiar symptom of nerve damage or diabetic neuropathy and it can be a troubling one. Caused by poor blood sugar control persisting over a period of time, neuropathy tends to be bilateral, meaning both feet may be affected and you will feel a loss of sensation when you touch or poke at them.
-
Tingling
Also caused by diabetic neuropathy, this feeling goes hand-in-hand with numbness and you may feel a heightened sensitivity to touch even when covering your feet with something light such as cloth. It could also transition from minor prickles to deep stabs of pain.
-
Muscle Weakness
As explained above, one of the causes of diabetic foot ulcers is the lack of blood supply to the nerves, which will subsequently affect the way your muscles move, leading to a lack of energy in your limbs. As reported in this study, because neuropathy usually affects muscle strength at the ankle of dorsal flexors and plantar flexors, you might experience difficulties in walking or standing.
-
Redness or Swelling
Foot ulcers can sometimes go undetected for some time and it may be too late once discovery is made. When you notice unusual swelling or redness, this is a clear indication that there is something wrong and you have injured your foot unknowingly. When this happens, make sure you take this seriously and not dismiss any possible symptoms early on.
-
Wounds and Ulcers
Infections are common in this condition as diabetic patients are more susceptible to open sores on the feet that are slow to heal, foul-smelling, or are draining due to impaired nerves and blood flow. When there is drainage, one may notice stains on one’s socks. These wounds or ulcers are usually unexplained and appear suddenly, hence should be examined and manageed as soon as possible.
While these symptoms may seem insignificant, they shouldn’t be ignored as they can be life-threatening.
Because of underlying nerve or vascular damage, infections that don’t seem to heal could develop to ulcers, and when not properly manageed, they could lead to foot deformities, amputation, and even death.
Prevention and Care Management
Here are some ways to control the occurrence of the aforementioned symptoms and developing ulcers:
- Reduce and eventually cease smoking habits to minimise smoking-induced oxidative stress, which may lead to ulcer development.
- Receive prompt care management of foot conditions such as dermatitis, cracked heels, and athlete’s foot before it worsens.
- Wear comfortable and properly fitted shoes to improve air circulation around the feet.
- Control your blood sugar and adhere to prescribed nutrition plans, which will reduce diabetic symptoms.
Getting educated about how to take care of foot and nail hygiene is crucial in reducing the risk of ulceration and preventing diabetic foot ulcers. If an ulcer has developed, never leave it to ‘dry out’ or be exposed to air.
It is essential to make sure the wound is cleaned thoroughly, use antiseptic, and apply a dressing. Avoid resting your weight on the affected area.
As soon as you can, arrange for an appointment to see a podiatrist who will be able to suggest and provide necessary care management during a consultation. Some care management options might involve skin and nail care for corns, calluses, or ingrown toenails.
One essential part of the care management process is to utilise pressure-relieving orthotic devices combined with diabetic-friendly footwear.
Some individuals may require custom footwear, TAG braces, soft or total contact casts, to offload pressure from the wound in more severe cases.
Failure to reduce load and pressure will result in the ulcer deteriorating and impede the healing process.
For advanced cases, ulcer debridement is conducted to remove unhealthy tissue from the wound. This will spark the body’s natural healing mechanism.
After the removal, a dressing will be applied to protect while the healing process takes place. In the aftercare phase, to aid in the speed of recovery, the patient should not apply unnecessary pressure to the affected area as it heals.
Get a Professional Consultation Today
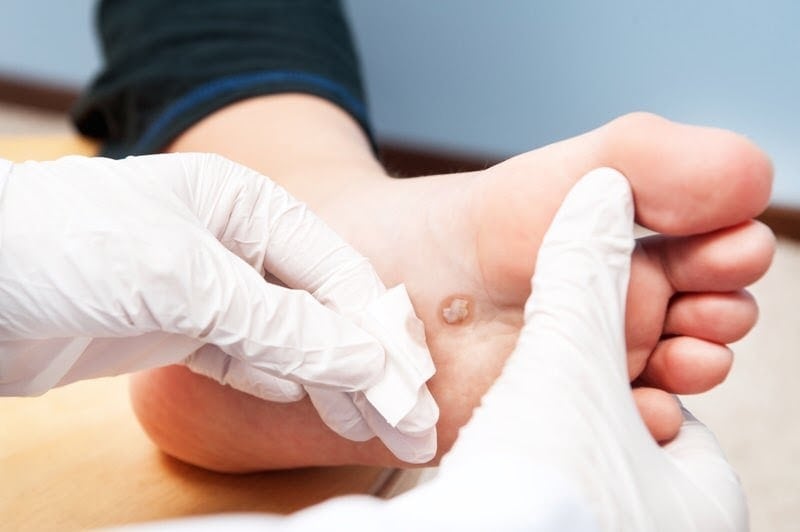
Diabetic foot ulcers may be difficult to diagnose as early-stage indications might seem too generic to be taken extra note of.
If you find something amiss during your daily inspections or would like to switch to custom-made insoles for your footwear, do pay a visit to your local podiatrist, My FootDr.
Contact us today to book an appointment and our professionals can determine if you are a high risk of developing a foot ulcer and guide you through preventive strategies.
